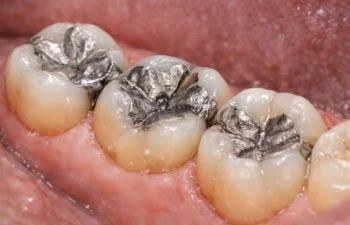
If you have older “silver” fillings, you’re not alone. Dental amalgam has been used for generations because it’s strong, durable, and cost-effective—especially on back teeth that take heavy chewing forces.
The #1 question we hear in our Alpharetta, Covington, Alpharetta, Sandy Springs, and Atlanta-area offices is:
“Should I remove my old amalgam (aka silver) fillings?”
Here’s our patient-first, evidence-informed answer: If an amalgam filling is stable and the tooth is healthy, routine removal is not recommended. Major dental and health authorities (including the ADA and FDA) state that available evidence does not show amalgam is harmful to the general population—and they do not recommend removing functioning fillings unless there’s a clinical reason (like decay, leakage, fracture, or pain).
At the same time, we also recognize a growing conversation—especially among functional/biologic-focused providers—about mercury exposure, individual sensitivity, and using extra safety steps when older fillings are replaced. That’s why our approach is balanced, transparent, and individualized.
What “stable” really means
A stable amalgam filling is one that:
- Feels comfortable when you bite or chew
- Shows no signs of cracks, chipping, or breakdown
- Has no evidence of decay around/under it on exam and X-rays
- Isn’t causing ongoing sensitivity, pain, or gum irritation
If that describes your filling, the most conservative—and often safest—choice is to monitor it at routine checkups instead of removing it “just because it’s old.”
The mainstream dental position (ADA/FDA-aligned)
Core point: The amount of mercury vapor released from amalgam is generally considered below levels shown to cause harm for most people, and large studies have not consistently shown systemic harm in the general population.
Why amalgam is still discussed as a valid material (historically and clinically):
- Durable, long-lasting performance
- Often cost-effective
- Particularly useful in posterior, load-bearing teeth and higher-caries-risk situations
Key takeaway:
- Safe for most people (per ADA/FDA statements)
- No blanket recommendation to remove existing amalgams if they’re in good condition
- Replacement should be based on clinical need, not fear
The mercury-toxicology / biologic dentistry perspective
Core point: Mercury is biologically active, and some practitioners argue that even low-dose exposure may matter for certain individuals—especially if they have heightened sensitivity or other risk factors.
This perspective emphasizes:
- Mercury is a known neurotoxin in other contexts and can cross the placenta
- Individual variability (genetics, detox pathways, immune sensitivity)
- Population studies can miss smaller subgroups who don’t respond “like the average person”
- A “precautionary principle” approach—especially for vulnerable groups
Our stance on this conversation:
We take patient concerns seriously, but we stay responsible with what we claim. We do not state that amalgam causes systemic diseases. Current mainstream guidance does not establish a direct cause-and-effect link for the general population.
However, we do agree on this: if replacement is needed or chosen, safety measures matter.
International and regulatory nuance (why the “phase down” is happening)
Globally, the trend has been to reduce (“phase down”) amalgam use, especially in children and in pregnancy-related groups. This shift is driven largely by environmental mercury concerns and public health precaution policies, alongside the availability of alternatives—not necessarily because there’s definitive proof of harm for all patients.
In fact, the Minamata Convention on Mercury addresses dental amalgam in the context of reducing mercury pollution.
When replacement is recommended
We don’t remove stable amalgams routinely, but there are clear reasons to replace them:
- Structural failure
If the filling is breaking down, wearing, or no longer sealing the tooth. - Recurrent decay (new decay around/under the filling)
If we diagnose decay at the margins or underneath, removing the filling and treating the decay is the right move. - Cracks or fractures
If the tooth is cracked or the filling is contributing to fracture risk, we may recommend an upgraded restoration (like an onlay or crown) depending on damage. - Esthetic concerns
If you want a more natural look, we can discuss tooth-colored options and the tradeoffs. - Patient preference—after informed consent
You always have a voice in your care. Our role is to explain benefits, risks, and alternatives so you can decide confidently.
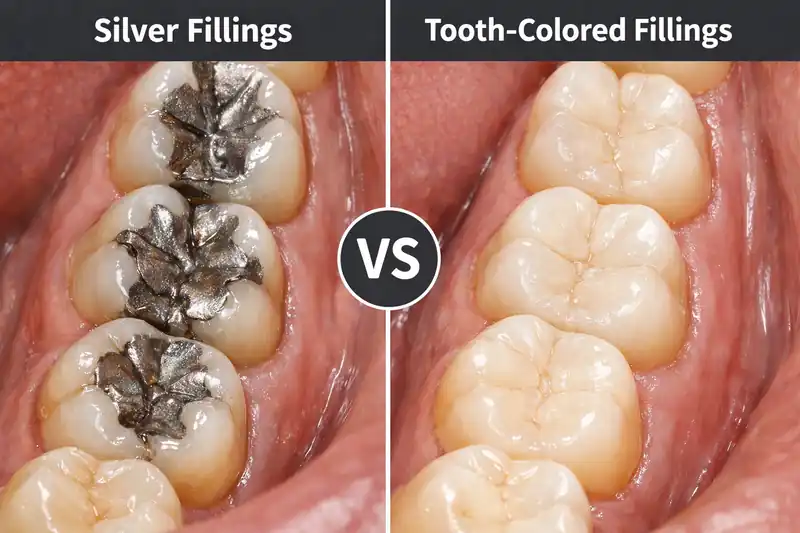
What we say (and don’t say) about mercury
- Yes, amalgam contains mercury as part of a stable alloy.
- Yes, the FDA notes that removing intact amalgam can temporarily increase mercury vapor exposure during removal, which is one reason they don’t recommend removal when fillings are in good condition.
- No, we don’t claim amalgam causes systemic diseases.
- Yes, the FDA has published recommendations that certain higher-risk groups may wish to avoid new amalgam when possible and appropriate.
Also, to be transparent: I personally don’t place mercury amalgam fillings anymore. When restoring teeth today, I prefer modern alternatives that fit the tooth, your bite, and your esthetic goals.
If we replace an old amalgam, we use extra safety measures
If replacement is truly needed—or if you choose it after reviewing pros/cons—we plan it carefully and use reasonable precautions, such as:
- Rubber dam isolation when appropriate
- High-volume evacuation/suction
- Controlled technique to reduce aerosol and exposure
- Thorough cleanup and aftercare guidance
We also focus on preserving healthy tooth structure and choosing a restoration that fits your goals (durability, appearance, longevity).
If you want a deeper overview, you may also like:
https://creativedentistryofatlanta.com/blog/dental-amalgam-fillings/
Bottom line
Old “silver fillings” aren’t “bad” by default. If they’re stable, we typically recommend monitoring—not automatically replacing. But if there’s damage, decay, fracture risk, esthetic concerns, or an informed personal preference, replacement can absolutely be the right choice—especially when done with modern materials and smart safety protocols.
If you’re in the Atlanta area (including Sandy Springs, Alpharetta, Roswell, Covington, and surrounding cities), schedule a visit so we can evaluate your fillings and talk through your best options.
Posted on behalf of Creative Dentistry & MedSpa

